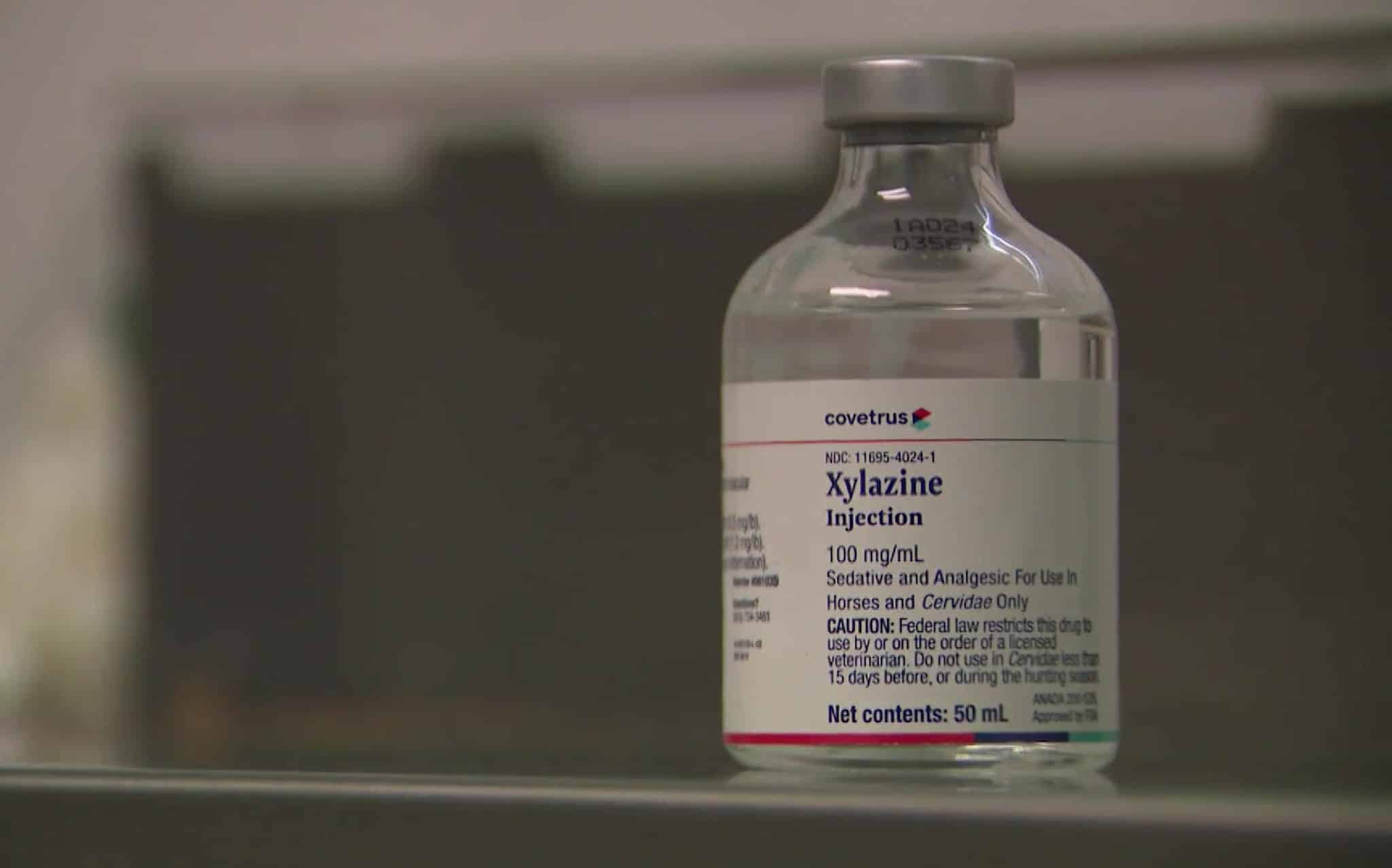
You may have heard of Xylazine making headlines in the news this past year, as it is becoming a popular drug laced with opioids, contributing to lethal overdoses. Xylazine makes fentanyl, the deadliest drug in the United States, even more fatal. The DEA Laboratory System is reporting that in 2022, approximately 23% of fentanyl powder and 7% of fentanyl pills seized by the DEA contained Xylazine.”
Xylazine is a non-opioid tranquilizer approved by the U.S. Food and Drug Administration for use in veterinary medicine and primarily used for sedation in large animal veterinary medicine. Also known as “Tranq,” Xylazine is not used or manufactured for human consumption as it is a central nervous system depressant. Over the years, it has been laced with opioids. Common side effects of Xylazine include sedation, difficulty breathing, low heart rate and blood pressure, and infected wounds, potentially leading to tissue necrosis, amnesia, and skin ulcerations. Because Xylazine is not regulated and relatively cheap, it is an attractive “cutting agent” for drug traffickers. While some individuals seek out xylazine-laced fentanyl or xylazine-laced heroin, believing that Xylazine prolongs fentanyl or heroin’s effects, others take it unknowingly.
“In 2022, provisional data indicated that more than two-thirds (68%) of the reported 107,081 drug overdose deaths in the United States involved synthetic opioids other than methadone, principally illicitly manufactured fentanyls (IMFs). Xylazine, a non-opioid sedative not approved for human use and with no known antidote, has been increasingly detected in IMF products in the U.S. drug supply* and in IMF-involved overdose deaths…it’s the increasing use (whether intentional or not) with fentanyl that caused the White House’s Office of National Drug Control Policy to declare the xylazine-fentanyl combination an “emerging threat to the United States” in April 2023”.
Is Xylazine addictive?
Xylazine is a non-opioid, and therefore, it does not share the addictive properties found in opioids such as morphine and fentanyl. However, because it is often laced with fentanyl, many falsely assume it can lead to addiction similar to opioids. There is insufficient evidence-based research to determine whether Xylazine can cause dependence and withdrawal. It is challenging to determine Xylazine’s risk of dependence and withdrawal since it is often laced with other drugs and is rarely consumed by itself.
Should I give Naloxone (Narcan) for a Xylazine overdose?
The intranasal version of naloxone is called Narcan, and it is administered during an opioid overdose as it blocks opioids from binding to their receptors, potentiating opioid withdrawal. In general, it is recommended that anyone suspected of experiencing an overdose, regardless of the drug, should be given naloxone. Naloxone only works in an opioid overdose; however, it does not hurt if given in other overdoses. It will not help, but it is not known to cause harm to the body. The school of thought is that many overdoses are associated with opioids, so it is better to err on safety and administer naloxone, which can potentially be life-saving in an opioid overdose. As a result, naloxone should be administered in a Xylazine overdose as Xylazine is usually laced with opioids. While naloxone will still effectively reverse opioid-induced respiratory depression and should be used as a life-saving treatment for any overdose that might involve opioids, as well as calling 911, the naloxone won’t reverse the effects of Xylazine. Thus, xylazine overdose may require additional supportive care, including maintaining an open airway, administering rescue breathing, and remaining with the individual until EMS arrives.